#opioids
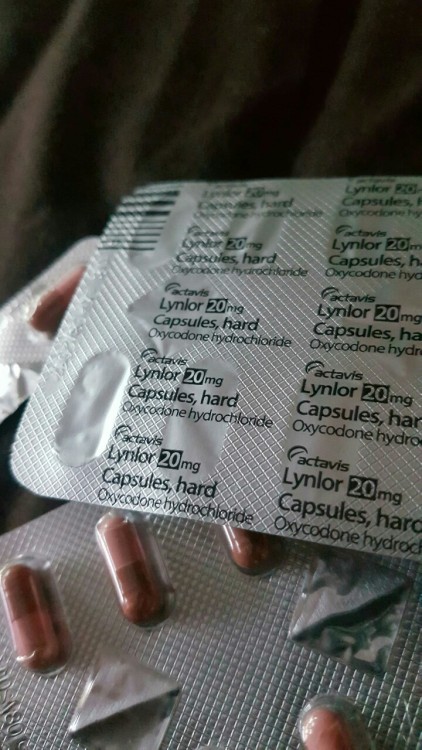
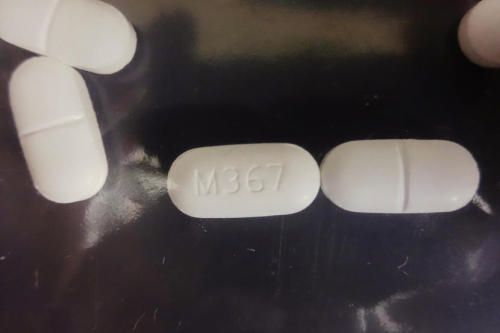
friendly reminder that opioids aren’t some profoundly dangerous thing. you’re literally ok to get them for surgery, procedures, etc. You won’t die if you take an extra one. Don’t deprive yourself of pain relief because of paranoid hysteria.
(the addiction rate is also very, very low)
I agree with the above post, but please exercise some caution with them. Even though the addiction rate is low, there still is a rate, so just stick with what youre prescribed and stick to recommended dose
Of course, always exercise caution when taking more than prescribed (I firmly reject the notion that that is in and of itself a key indicator of addiction, I’m a sentient human being who knows there is a tangible effect with my pain medicine and have transient pain that can’t just follow verbatim instructions) but in general people do not have to endure suffering because they’re aggressively paranoid about addiction.
The strongest risk factors for addiction are preexisting mental health conditions but especially prior substance misuse (well, abuse, but that term is less preferred because it’s stigmatizing but I think it explains the idea better — misuse to the point of acute harm) and socioeconomic determinants of health that reinforce drug use as a coping mechanism. Dose, duration, specific opioid are all much less predictive of addictive risk.
An overwhelming majority of “accidental addicts” actually weren’t all that accidental.
And as far as the most extreme outcome, fatal overdose, that’s just simply not likely unless you’re being ultra silly. The LD50 of morphine is estimated to be about 150-250mg. That is equal to about 30-50 standard (5mg) Vicodin (1.0x conversion factor for hydrocodone) or 10-17 highest strength (10mg) Percocet (1.5x conversion for oxycodone).
[HARM REDUCTION] And please god if you are going to enjoy a recreational dose of them (no judgement here) please avoid concomitant use of alcohol and/or benzodiazepines. Potentiation gets people killed if you underestimate it. Neither is likely to kill you by themselves without a very irresponsibly large dose, but together the risk profile grows dramtically. If using multiple CNS depressants, cut all doses. Obvious harm reduction recommendations of start low, go slow also apply.
VICTORY! California Governor Newsom just signed the state budget, officially allocating $15.2 million to fund staff positions in syringe service programs across the state!
Over the last two years Harm Reduction Coalition talked with programs & PEOPLE who use drugs to understand what was needed to truly reduce the health & social harms of drug use, & we kept hearing one thing: more people to do the work! People across the state came together to advocate for this budget ask, led by Drug Policy Alliance & Harm Reduction Coalition. It was a collaborative effort from the beginning to today’s victory!
Post link
The latest Narcotica podcast sits down down with Harm Reduction Coalition’s, Eliza Wheeler. Eliza has been working in harm reduction, distributing syringes & naloxone directly to people who use drugs for over two decades, & reflects on how easily the bedrock values and principles of the movement can be compromised and co-opted by political forces when it goes mainstream. Eliza talks about how funds for naloxone end up in the wrong hands, how syringe access deals with NIMBYism, & how the heart of her harm reduction philosophy is bodily autonomy.
Post link
CALL TO ACTION! California legislators will soon be doing the final vote on a budget proposal that would fund a paid staff position in all authorized syringe access programs!
We need your help pushing it through, please call the Senators and Assemblymember’s on the Budget Conference Committee:
- Assemblymember Phil Ting (SF) (415) 557-2312
- Senator Richard Roth (Riverside) (951) 680-6750
- Senator Nancy Skinner (Alameda) (510) 286-1333
- Senator Holly Mitchell (LA) (213) 745-6656
Here’s a sample of what you could say:
“Hi, my name is ______ and I live/work in _____. I’m calling to ask ___[name of legislator]___ to support the budget request led by Harm Reduction Coalition and Drug Policy Alliance to fund Harm Reduction Care Navigators.
This is important because syringe service programs are on the front lines providing care to people who need it most and many of these programs have little money or are all volunteer. These funds would make it possible to help connect people to treatment and reduce overdose deaths in California. Please support this budget request!”
Post link
Save the Date: 13th National Harm Reduction Conference, San Juan, Puerto Rico, October 17-20, 2020
Post link

Do you know aboutfentanyl? Fentanyl is a powerful opioid that has been found in heroin, cocaine, crack, methamphetamine, ketamine and pills from nonmedical sources. Anyone who uses drugs that may contain fentanyl, even occasionally, may be at risk of overdose.
The presence of fentanyl in the New York City drug supply has dramatically increased the number of overdose deaths, and fentanyl is now the most common drug involved in overdose deaths. In 2020, 1,580 New Yorkers died from a fentanyl-involved overdose.
To prevent an overdose:
Avoid using alone and take turns.
Start with a small dose and go slowly.
Keepnaloxone ready and on hand. Call 311 to find out where to get naloxone at no cost.
Avoid mixing drugs.
Test your drugs using fentanyl test strips
As a pain specialist, I may have caused more harm by underprescribing opioids
A reporter recently asked me about what harm I may have caused as a pain management physician who prescribes opioids. As I reflected on my last 10 years in this field, my response was that the harms I may have caused were because I underprescribed these drugs, not overprescribed them.
I thought of a 25-year-old patient, I’ll call him John, whose sciatic nerve was crushed in a motor vehicle accident, causing excruciating pain in his leg. We knew this would be a life-long injury, and that he would likely have to live with chronic pain. We tried everything I could think of — nerve medications, mindfulness techniques, desensitization, rehabilitation techniques, cognitive therapy, nerve blocks, and spinal cord stimulation — except opioids. John continued to suffer immensely from the debilitating pain, and eventually died by suicide.
Did he die because I undertreated his pain due to my own fear of prescribing chronic, potentially high-dose opioids in a young patient? I cannot know, but I worry and fear that this may be true.
In 2016, the Centers for Disease Control and Prevention published prescribing guidelines for opioids. Though intended to encourage best practices in opioid prescribing, these guidelines fueled providers’ fears of opioids and led to many clinicians abandoning patients who relied on opioids for pain relief. Although even pain specialists like me share fears and doubts about what role these medications play in managing chronic pain, so-called legacy patients are not the same as those who have never taken opioids before, as a colleague and I explained in The New England Journal of Medicine. (Read more at link)
Here’s a fascinating study. A pair of researchers at the University of Georgia took a look at what happened to prescriptions for opioid painkillers in states that passed medical marijuana laws. Over at the Washington Post, Christopher Ingraham summarizes their results:
They found that, in the 17 states with a medical-marijuana law in place by 2013, prescriptions for painkillers and other classes of drugs fell sharply compared with states that did not have a medical-marijuana law. The drops were quite significant: In medical-marijuana states, the average doctor prescribed 265 fewer doses of antidepressants each year, 486 fewer doses of seizure medication, 541 fewer anti-nausea doses and 562 fewer doses of anti-anxiety medication.
Needless to say, the painkiller industry would much rather have you gulp down their addictive and lucrative product. They are not taking the threat from medical marijuana lying down:
The tanking numbers for painkiller prescriptions in medical marijuana states are likely to cause some concern among pharmaceutical companies. These companies have long been at the forefront of opposition to marijuana reform, funding research by anti-pot academics and funneling dollars to groups, such as the Community Anti-Drug Coalitions of America, that oppose marijuana legalization.
Pharmaceutical companies have also lobbied federal agencies directly to prevent the liberalization of marijuana laws. In one case, recently uncovered by the office of Sen. Kirsten Gillibrand (D-N.Y.), the Department of Health and Human Services recommended that naturally derived THC, the main psychoactive component of marijuana, be moved from Schedule 1 to Schedule 3 of the Controlled Substances Act — a less restrictive category that would acknowledge the drug’s medical use and make it easier to research and prescribe. Several months after HHS submitted its recommendation, at least one drug company that manufactures a synthetic version of THC — which would presumably have to compete with any natural derivatives — wrote to the Drug Enforcement Administration to express opposition to rescheduling natural THC, citing “the abuse potential in terms of the need to grow and cultivate substantial crops of marijuana in the United States.”
The study estimates that if all 50 states legalized medical marijuana, Medicare would save $500 million per year in painkiller spending. It’s hard to extrapolate that to overall spending on painkiller medication, but the total savings would be on the order of $2 billion per year—maybe more.
Post link
Fentanyl is the strongest opioid approved for medical use in the United States, rated as 30 to 50 times more potent than heroin.
Here’s the deadly history of the drug that killed Prince.
Post link
It was 10 years ago today that I looked down at the pills laid out in front of me and made a life-altering decision. I had been trying for months to scale back, ween myself, anything I could to get off of the pills. I talked to someone in my family who had gone through something similar for advice. But no matter what I did, I just seemed to keep digging myself into a bigger hole. I couldn’t call my doctor out of fear of being blacklisted for any future medications that I might, and most definitely would, need as my degenerative disease got worse. But I needed to do something. I *had* to do something. I was staring down a very black hole.
On this day 10 years ago a little voice inside of me spoke up and told me that the next choice I made was going to be between my future and my end. My life and my death. And so I chose.
I chose Life.
Today is my 10 years sober.
Genetic Signals Linked to Problematic Opioid Use
UC San Diego School of Medicine researchers asked more than 132,000 23andMe research participants of European ancestry “Have you ever in your life used prescription painkillers, such as Vicodin and Oxycontin, not as prescribed?” More than 21 percent said yes. Then, in a genome-wide association study, the team discovered novel genomic regions that influenced using opiate drugs not as prescribed. They also identified strong genetic correlations with other substance use traits, including opioid use disorder.
The study, published November 2, 2021 in Molecular Psychiatry, was led by Sandra Sanchez Roige, PhD, and Abraham Palmer, PhD.
Post link
The U.S. government’s current strategy of trying to restrict the supply of opioids for nonmedical uses is not working. While government efforts to reduce the supply of opioids for nonmedical use have reduced the volume of both legally manufactured prescription opioids and opioid prescriptions, deaths from opioid overdoses are nevertheless accelerating. Research shows the increase is due in part to substitution of illegal heroin for now harder-to-get prescription opioids. Attempting to reduce overdose deaths by doubling down on this approach will not produce better results.
Policymakers can reduce overdose deaths and other harms stemming from nonmedical use of opioids and other dangerous drugs by switching to a policy of “harm reduction” strategies. Harm reduction has a success record that prohibition cannot match. It involves a range of public health options. These strategies would include medication-assisted treatment, needle-exchange programs, safe injection sites, heroin-assisted treatment, deregulation of naloxone, and the decriminalization of marijuana.
Though critics have dismissed these strategies as surrendering to addiction, jurisdictions that have attempted them have found that harm reduction strategies significantly reduce overdose deaths, the spread of infectious diseases, and even the nonmedical use of dangerous drugs.
Just agreed to do research surveys since just sitting here waitin, but 1st 1 about opioids I take & now sweatin wondering if I shoulda put that shit on file, which is ridic bc already in my med file but this is more accessible to outside sources idk.