#immunology
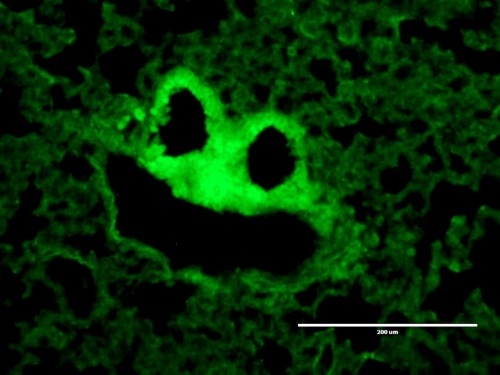
Spooky science
This ghoulish image shows lung tissue structure.
Laura Sibley who took this image is part of a team from Royal Holloway, who are developing novel vaccines using bacteria (similar to ones that are used in probiotic drinks).
The vaccines they are creating are cheaper than normal vaccines, easier to produce and have no chemicals in them, making them suitable for diseases affecting developing countries. There are many diseases that need vaccine development, including tuberculosis, which kills around two million people per year, and is one of the diseases that they are focused on.
Laura stumbled across the ghostly vision in a study looking at TB vaccine distributed in lung tissue, work which in the future could help to protect people against TB infection.
Post link
Multiple allergic reactions traced to single protein
Johns Hopkins and University of Alberta researchers have identified a single protein as the root of painful and dangerous allergic reactions to a range of medications and other substances. If a new drug can be found that targets the problematic protein, they say, it could help smooth treatment for patients with conditions ranging from prostate cancer to diabetes to HIV. Their results appear in the journal Nature on Dec. 17.
Previous studies traced reactions such as pain, itching and rashes at the injection sites of many drugs to part of the immune system known as mast cells. When specialized receptors on the outside of mast cells detect warning signals known as antibodies, they spring into action, releasing histamine and other substances that spark inflammation and draw other immune cells into the area. Those antibodies are produced by other immune cells in response to bacteria, viruses or other perceived threats. However, “although many of these injection site reactions look like an allergic response, the strange thing about them is that no antibodies are produced,” says Xinzhong Dong, Ph.D., an associate professor of neuroscience in the Institute for Basic Biomedical Sciences at the Johns Hopkins University School of Medicine.
To zero in on the cause of the reactions, Benjamin McNeil, Ph.D., a postdoctoral fellow in Dong’s laboratory, first set out to find which mast cell receptor — or receptors — responded to the drugs in mice. Previous studies had identified a human receptor likely to be at fault in the allergic reactions; McNeil found a receptor in mice that, like the human receptor, is found only in mast cells. He then tested that receptor by putting it into lab-grown cells and found that they did react to medications that provoke mast cell response. He found similar results for the human receptor that previous studies had indicated was a likely culprit.
“It’s fortunate that all of the drugs turn out to trigger a single receptor — it makes that receptor an attractive drug target,” McNeil says.
Post link


immunology notes | 04.11.20
I hope everyone is doing well during the quarantine period! I’ll be answering my backlog of asks here tonight :)
you can follow my studygram (studyingdoc) because I find it easier to be active there hehe
Taking daily vitamin D supplements — or a combination of vitamin D and omega-3 fish oil — appears to carry a lower risk of developing autoimmune disease, with a more pronounced effect after two years, finds a trial of older US adults published by The BMJ.
The researchers say the clinical importance of these findings is high, “given that these are well-tolerated, non-toxic supplements, and that there are no other known effective therapies to reduce rates of autoimmune diseases.”
Autoimmune disease happens when the body’s natural defense system mistakenly attacks normal cells. Common conditions include rheumatoid arthritis, psoriasis, and thyroid diseases, which increase with age, particularly among women.
Researchers set out to test the effects of vitamin D and omega-3 fish oil supplements on rates of autoimmune diseases in 25,871 US adults.
Autoimmune disease was reduced by 22% in those who took the increased levels of Vitamin D with or without fish oil. And those that only took fish oil supplements saw disease decline of 15%. More research is needed to better understand the effects of dietary supplements on autoimmune disease, like lupus.
A 57-year-old man with life-threatening heart disease has received a heart from a genetically modified pig, a groundbreaking procedure that offers hope to hundreds of thousands of patients with failing organs.
It is the first successful transplant of a pig’s heart into a human being. The eight-hour operation took place in Baltimore, and the patient, David Bennett Sr. of Maryland, was doing well three days later, according to surgeons at the University of Maryland Medical Center.
Researchers say they have found a second patient whose body seemingly had rid itself of the human immunodeficiency virus (HIV) that causes AIDS — supporting hope that it may be possible someday to find a way to cure more people of the virus.
Joan A. Steitz (b. 1941) is a biologist whose research focused on RNA and its interaction with ribosomes, for which she won the Lasker-Koshland Award for Special Achievement in Medical Science.
She obtained her PhD from Harvard and conducted postdoctoral research at the University of Cambridge. Her research offered groundbreaking insight into autoimmune diseases, their causes and treatments. She is a Professor of Molecular Biophysics and Biochemistry at Yale University.
Post link
““When we challenge dogma we no longer get burned at the stake, which is helpful.””— Immunology lecturer

Cover art for my thesis:
Immune-system-on-a-chip: future perspectives on in vitro immune tissue culture
Opinion: Why science needs philosophy
By Lucy Laplane, et. al.
Despite the tight historical links between science and philosophy, present-day scientists often perceive philosophy as completely different from, and even antagonistic to, science. We argue here that, to the contrary, philosophy can have an important and productive impact on science.
Post link
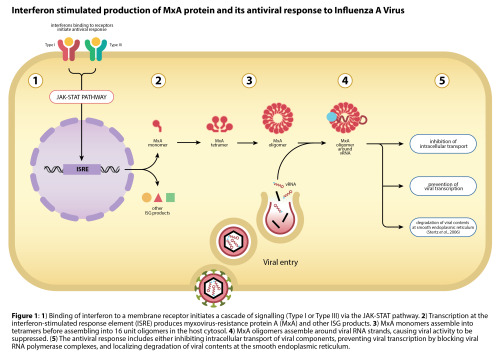
Interferon stimulated production of MxA protein and its antiviral response to Influenza A Virus | December 2015
A simplified immunological illustration signifying the production of MxA protein via interferon signalling and its method of attack against influenza.
Note: most literature today is unclear of the precise degradation pathways MxA takes with removing viral contents from a host cell.
Post link
Hepatitis A Vaccination Required for Herd Immunity in People Experiencing Homelessness or Who Use Drugs
In the U.S., hepatitis A outbreaks are repeatedly affecting people experiencing homelessness or who use drugs. A 2017-19 Kentucky outbreak primarily among these groups resulted in 501 cases, six deaths. Vaccination efforts likely averted 30 hospitalizations and $490K in costs, but UC San Diego and Oxford researchers say more could have been saved if initiated earlier and faster. They determined herd immunity in these populations requires 77 percent vaccinated, underscoring need for outreach.
The study, published October 18, 2021 in Vaccine, was led by Natasha Martin, DPhil, professor at UC San Diego School of Medicine, and Emmanuelle Dankwa and Christl Donnelly, CBE FMedSci FRS, at University of Oxford.
Pictured: A UC San Diego Health employee is vaccinated against hepatitis A during an outbreak in San Diego, Calif. in 2017. Credit: Erik Jepson/UC San Diego Publications
— Heather Buschman, PhD
Post link
Coronavirus be like, “I’m viral.”
PS: Don’t be a victim of mass hysteria.
What are your thoughts on the coronavirus?
Post link
Exercise 1.1
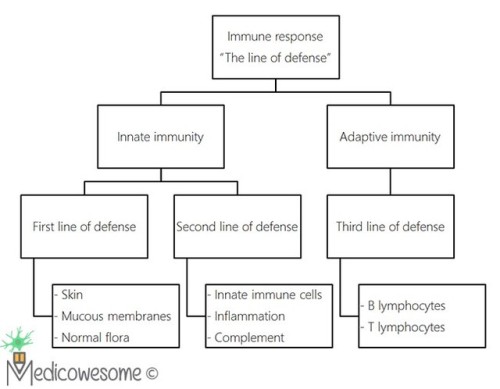
Which components of the immune system do the following belong to - innate or adaptive?
1. Lysozyme
2. Natural Killer cells
3. T lymphocytes
4. Epidermis
5. Fever
6. Antigen presenting cell
7. Interferon
8. Plasma cells
9. Complement
10. Toll like receptors
11. Vomiting
Post answers below!
You can give back to us if you like our content by:
1. Using PayPal
Donate with PayPal button
PayPal supporters will receive a printable pdf (I will try to send it asap if you request it, but then again, I am a resident and super busy so may not be able to get back to you!)
2. Supporting the authors website by visiting and sharing the page!
VisitmedXclusive.org by Bobby V. Shirke
Visitmedicowesome.com by Nakeya Dewaswala
Post link
Hello everyone,
As you guys probably already know - my co-author, Bobby V. Shirke, and I were working on a book, Immunowesome. We finished writing the book a while ago and we planned to publish it and sell it on Amazon Kindle for a few dollars. However, we were so busy that we stopped after finishing the book and receiving copyright.
So today, we decided that instead of letting the book sit in my computer and collect (binary) dust, we will release it for free on Immense Immunology Insight :)
You can give back to us if you like our content by:
1. Using PayPal
Donate with PayPal button
PayPal supporters will receive a printable pdf (I will try to send it asap if you request it, but then again, I am a resident and super busy so may not be able to get back to you!)
2. Supporting the authors website by visiting and sharing the page!
VisitmedXclusive.org by Bobby V. Shirke
Visitmedicowesome.com by Nakeya Dewaswala
Releasing cover page and contents page today as a teaser :D
- IkaN
Post link
1. Mycobacterium tuberculosis - Stops fusion!

Mycobacterium tuberculosis utilizes macrophages for its replication! (It uses the usual killer to expand it’s army :O ) How does tuberculosis bacilli survive in macrophages? M. tuberculosis has evolved a number of very effective survival strategies - It inhibits phagosome-lysosome fusion and inhibits phagosome acidification ensuring it’s survival inside the macrophage.
2. Brucella - Has chains, like Bruce Lee.

Brucellahas a LPS O-chain. It ensures the Brucella containing vacuole (BCV) avoids fusion with lysosomes, prevents the deposition of complement at the bacterial surface and forms stable large clusters with MHC-II named macrodomians in the cell surface, interfering with MHC-II presentation of peptides to specific CD4+ T cells. Woah.
3. Listeria - It gets internalized in a vacuole and then runs away.

The pore-forming protein listeriolysin O mediates escape from host vacuoles. Once in the cytosol, the L. monocytogenes mediates efficient actin-based motility, thereby propelling the bacteria into neighboring cells. The cytosol is a favorable environment for listeria’s growth.
4. Mycobacterium leprae - Cholesterol and TACO!

Mycobacterium leprae is able to induce lipid droplet formation in infected macrophages. Cholesterol mediates the recruitment of TACO from the plasma membrane to the phagosome. TACO, also termed as coronin-1A (CORO1A), is a coat protein that prevents phagosome-lysosome fusion and thus degradation of mycobacteria in lysosomes. The entering of mycobacteria at cholesterol-rich domains of the plasma membrane and their subsequent uptake in TACO-coated phagosomes promotes intracellular survival.
5. Coxiella brunetti - The indestrucible

This hardy, obligate intracellular pathogen has evolved to not only survive, but to thrive, in the harshest of intracellular compartments: the phagolysosome. Following internalization, the nascent Coxiella phagosome ultimately develops into a large and spacious parasitophorous vacuole (PV) that acquires lysosomal characteristics such as acidic pH, acid hydrolases and cationic peptides, defences designed to rid the host of intruders.
6. Salmonella - TTSS

Salmonella have a specialized secretion system, termed the type III secretion system (TTSS), as well as proteins secreted by this system, are encoded in Salmonella pathogenicity island 1 (SPI1). TTSS are used by bacterial pathogens to inhibit their phagocytosis, induce eukaryotic cell death, and alter the host cell cytoskeleton. Salmonella species have at least one other TTSS encoded on SPI2 that appears to be involved in intracellular survival.
7. Human Immunodeficiency Virus - Tries to not attract attention

After infecting cells, HIV survives. Ever wondered why? It’s because the HIV protein, Nef plays a role in downregulating the expression of various proteins needed for recognition by potentially dangerous CD8 T cells. Nef lowers the surface expression of CD4, and several haplotypes of MHC-I by redirecting their transport from the trans-Golgi network. Another gene, Tat, appears to upregulate the expression of Bcl-2 during the early phase of cellular infection, increasing the likelihood that it will receive survival signals.
Many viruses can survive intracellularly, but I’ve included specifically HIV in this list because it survives in immune cells and it is an important virus to know.
The fourth type of ELISA is competitive ELISA. As the name suggest there is going to be a competition between someone. Now let’s see between whom is this competition exactly going to be.
Let’s take an example wherein we have to detect HIV antibodies from a serum sample.
For detection of HIV antibodies, the wells of micro titre plate are coated with HIV antigen followed by incubation of antibodies from the sample. After incubation detection antibodies specific to HIV antigens are added.
Now, if the sample contains HIV antibodies then antigen-antibody complexes are formed. No antigen is left for detection antibody to bind.
Hence, these detection antibodies remain free and are washed off. Addition of substrate to such a well gives no colour change indicating a positive result.
On the other hand, if the sample does not contain HIV antibodies then there is no antigen-antibody complex formed. Thus, the detection antibodies bind to the antigen which will show a colour change on addition of substrate indicating a negative result.
Thus, competitive ELISA involves a competition between detection antibody and sample antibody to bind with the sample antigen.
Also, in other types of ELISA colour change detected a positive result and no colour change detected a negative result whereas in competitive ELISA it’s exactly opposite!
Post link
The contents page! Yaay!
All about cells in the immune system
Monocytes & macrophages simplified
Natural killer cells simplified
- The chronicles of the T cell and B cell
Thymus dependent activation of B lymphocytes simplified
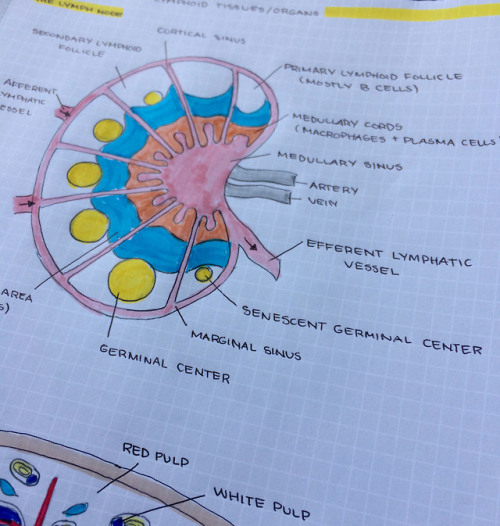
Where do B cells and T cells reside in the lymph nodes and spleen?
Function of B lymphocyte simplified
Function of Cytotoxic T lymphocyte simplified
Why is B cell called a B cell?
Immunology basics
- Interleukins
Which interleukins are secreted by T cells? (Mnemonic)
- Major Histocompatibility Complex
Which cells have which MHC class?
Antigen presenting cells display processed antigens to T cells through which MHC molecule?
Immuno-pharmacology
How do anti-TNF biologics work?
Other
Immune system has 2 arms - Innate and Adaptive
Ciliated epithelial cells - A physical barrier of the immune system
Antibodies and antigens
What is the difference between immunogenicity and antigenicity?
Functions of antibodies simplified
- Immunology in diagnostics
ELISA: Enzyme Linked Immuno Sorbent Assay
Enzyme-linked immunosorbent assay (ELISA) simplified
Immunological disorders
Question: What happens when mother is Rh positive and fetus is Rh negative?
- Neoplasia, cancer and tumors
Hairy cell leukaemia simplified
7 reasons why cancer cells are immortal
- Autoimmune diseases
What happens in type 1 diabetes mellitus?
Once you get an autoimmune disease, you are more likely to get others. Why?
Systemic Lupus Erythematosus and related antibodies
- Hypersensitivity
Stages of delayed type of hypersensitivity simplified
- Immunodeficiency disorders
- Transplantation immunology
Why are transplanted organs rejected?
Bacteriology
Teaching immunology to kids: We are friends with bacteria
Cell wall of gram positive and gram negative bacteria mnemonic
Random giggles
- Neuron pencil
- A molecular minute
Catecholamines and the immune system
- Totally comics
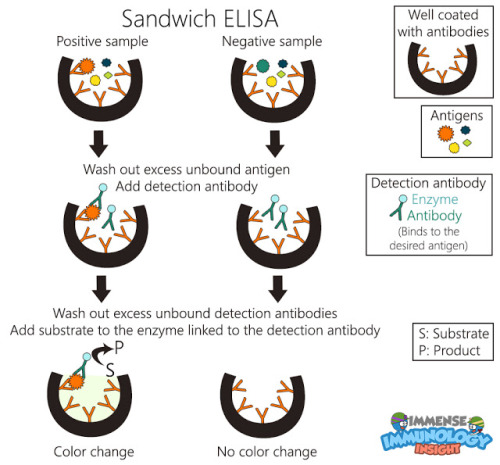
To remember this type of ELISA, imagine a sandwich! The antigen is the filling and the antibodies are the yummy bread. Hungry, aren’t you?
In this type of ELISA, an antibody of a particular antigen is adsorbed to the walls of well.
Then sample antigens are added.
If the sample contains desired antigen it will bind to the antibody.
After the unbound antigens are washed off, detection antibodies which bind specifically to desired antigen are added.
Unbound detection antibodies are washed off followed by substrate addition.
Sample containing bound detection antibody will give colour change indicating the presence of antigen and the sample which do not have any bound detection antibody will be colourless.
Post link
Indirect ELISA is used for detection of a particular antibody in a given sample. Most of the HIV diagnosis kits use indirect ELISA principle.
In this type of ELISA, the antigen (viral coat in case of HIV) are adsorbed to the walls of well.
Antibodies from patient are then added to the well.
If the patient is HIV positive he will produce antibodies against the HIV antigen and if he is HIV negative, there won’t be any antibodies against the antigen.
After that, detection antibodies which will recognize human antibodies are added.
The unbound detection antibodies are washed off followed by substrate addition.
If the sample contains antibodies against HIV, it will show a colour change due to the detection antibody bound to it.
If the sample is HIV negative, it won’t show ant colour change as it does not have any bound detection antibody.
Post link
ELISA: Enzyme Linked Immuno Sorbent Assay
From pregnancy detection kits to HIV diagnosis it is ELISA which gives us appropriate results.
Though ELISA has got a complex name, the way in which it diagnosis is really simple!
ELISA is performed in special micro titre plates which has wells in which we add our sample and then perform ELISA.
There are 4 types of ELISA:
- Direct
- Indirect
- Sandwich
- Competitive
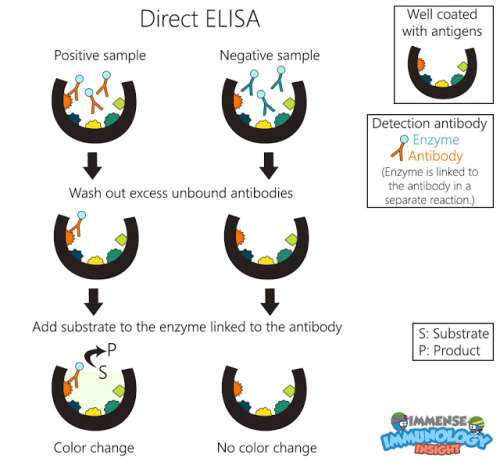
Direct ELISA is performed by attaching the sample antigens on a surface (walls of wells) then a specific antibody is applied so that it can bind to its corresponding antigen.
The antibodies used in ELISA are special they are known as Detection antibodies. These antibodies have an enzyme linked on its surface. The detection antibody being specific for a particular antigen it will bind only if that particular antigen is present in the sample. After applying antibodies the next step is to wash off the unbound antibodies.
Now, there are 2 possibilities
1. The sample is positive for a particular antigen: In this case it will have detection antibodies bound to it. The sample is then treated with the substrate of enzyme linked to the detection antibody. The enzyme converts the substrate into a product which will give a colour change.
Now this colour change is directly proportional to the amount of antigen present in the given sample.
2. The sample is negative for a particular antigen: In this case, all the detection antibodies will be washed off as the specific antigen is absent. The enzyme bound to the detection antibody will also be lost. Hence, when substrate is added it will not be converted into product giving us no colour change.
This is how ELISA works!
I’ll explain indirect and sandwich ELISA in my next blog. So stay tuned! :)
The image was hand-drawn and submitted to us by Komal M Kadam. You can submit your notes too by mailing it to us at [email protected]
Post link
Alocal police encounters a most wanted criminal and puts him behind bars. The criminals’ information is now sent to the FBI for further investigation. It is the FBI which will take appropriate actions against the criminal.
Now, imagine the criminal is the antigen which has been encountered by a cell - local police. The cell represents a part of antigen - criminals information on their cell surface so that the T-cells - the FBI can identify the antigen and destroy it!
T-cells can bind to only those antigens which are present on cell membrane proteins called Major histocompatibility complexes. The FBI can trust the police only if they come with a badge.
There are 2 class of these MHC Complexes :
• Class I (present on the surface of nucleated cells)
• Class II (present on the surface of Antigen Presenting Cells)
Also, there are 2 major types of T-cells:T-Helper cellsandT-Cytotoxic cells.
The TH-cells recognizes antigens on MHC Class II Complex present only on Antigen Presenting Cells and TC-cells cells recognizes antigens on MHC Class I Complex present only on Nucleated cells.
Post link
Thethymus is a specialised primary lymphoid organ of the immune system.
- At its largest and most active during the neonatal and pre-adolescent periods.
- Decreases in size and activity through teenage years
- Thymus tissue is gradually replaced by adipose tissue(fat).
- Residual T lymphopoiesis continues throughout adult life.
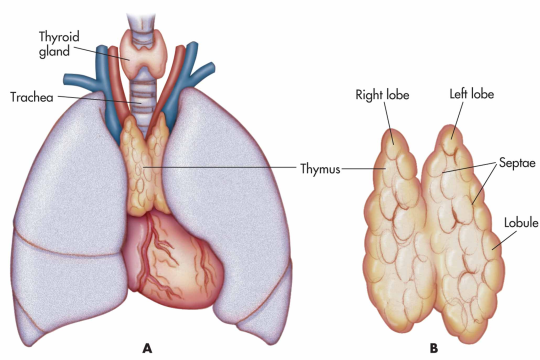
The thymus is composed of two identical lobes and is located in the anterior superior mediastinum, in front of the heart and behind the sternum. Each lobe of the thymus can be divided into a central medulla and a peripheral cortex which is surrounded by an outer capsule.
Function
Facilitates the maturation of T cells - which provide cell-mediated immunity.
- T cells begin as hematopoietic precursors from the bone-marrow, and migrate to the thymus, where they are referred to as thymocytes.
- In the thymus they undergo a process to ensure the cells react against antigens (“positive selection”), but that they do not react against antigens found on body tissue(“negative selection”).
- Once mature, T cells emigrate from the thymus to provide vital functions in the immune system.
- Each T cell has a distinct T cell receptor, suited to a specific substance, called an antigen.
- Most T cell receptors bind to the major histocompatibility complex on cells of the body.
Positive selection
T cells have distinct T cell receptors. These are formed by process recombination gene rearrangement which is error-prone, and some thymocytes fail to make functional T-cell receptors, whereas other thymocytes make T-cell receptors that are autoreactive. The survival and nature of the T cell then depends on its interaction with surrounding thymic epithelial cells.
- T cell receptor interacts with the MHC molecules on the surface of epithelial cells.
- A T cell with a receptor that doesn’t react, or reacts weakly will die by apoptosis.
- A T cell that does react will survive and proliferate.
- A mature T cell expresses only CD4 or CD8, but not both.
Negative selection
T cells that attack the body’s own proteins are eliminated in the thymus. Epithelial cells in the medulla and dendritic cells in the thymus express major proteins from elsewhere in the body. Some CD4 positive T cells exposed to self antigens persist as T regulatory cells.
Pathology
Immunodeficiency - As the thymus is the organ of T-cell development, any congenital defect in thymic genesis or a defect in thymocyte development can lead to a profound T cell deficiency in primary immunodeficiency disease.
Autoimmune disease - Genetic disorders, such as Myasthenia gravis: caused by antibodies that block acetylcholine receptors.
Thymomas - Originate in thymic epithelial cells most often in adults older than 40. Generally detected when they cause symptoms, such as a neck mass or affecting nearby structures such as the superior vena cava. Can be benign; benign but by virtue of expansion, invading beyond the capsule of the thymus (“invasive thyoma”), or malignant (a carcinoma).
Lymphomas - Tumours originating from T cells of the thymus form a subset of acute lymphoblastic leukaemia (ALL)
Thymic cysts - The thymus may contain cysts, usually less than 4 cm in diameter. Thymic cysts are usually detected incidentally and do not generally cause symptoms.